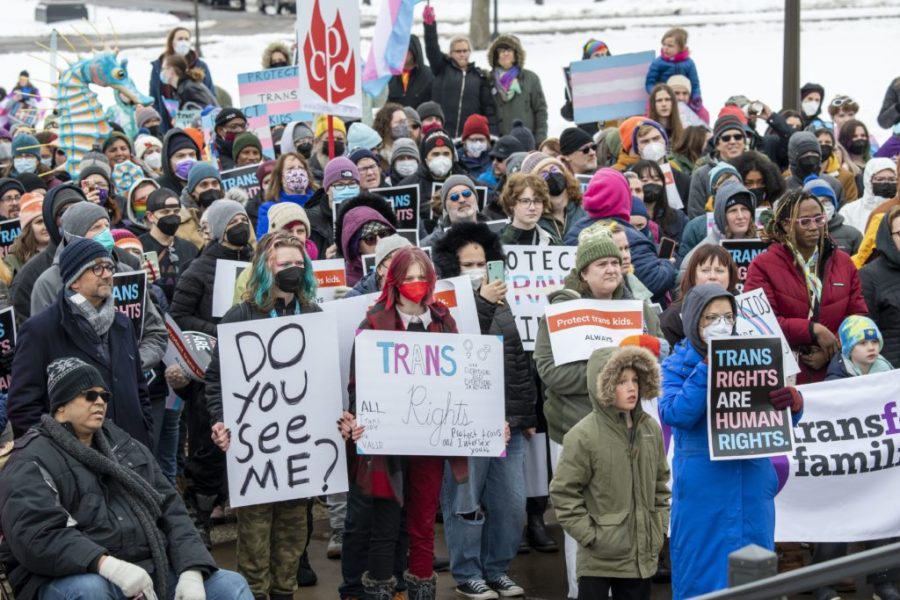Transgender Nebraskans face inequality in physical, mental healthcare access
Author’s Note: Some of the sources referenced in this piece requested to remain anonymous due to personal fears about sharing their experience as trans individuals, which is why certain sources have their names redacted. This article contains transphobic content.
UCG/Universal Images Group via G
St. Paul, Minnesota. March 6, 2022. Because the attacks against transgender kids are increasing across the country Minneasotans hold a rally at the capitol to support trans kids in Minnesota, Texas, and around the country. (Photo by: Michael Siluk/UCG/Universal Images Group via Getty Images)
LGBTQ+ individuals living in rural Nebraska have many barriers stopping them from getting proper physical or mental healthcare, according to OneWorld.
Melanie Budine, a Nurse Practitioner and teen/young adult healthcare provider at OneWorld explains that there is no clinic that offers transgender hormone therapy west of 130th street in Omaha. She explained how her clinic sees a lot of patients from western Nebraska.
“Before I was at OneWorld I was at a nonprofit that was called Associates of Reproductive Healthcare,” Budine said. “It was just for transgender care. That was in Bellevue. At that location, I had patients coming from all over western Nebraska and Central Iowa, but even at OneWorld I have one patient who is out at Chadron.”
The drive from Chadron, NE to 130th and Center, the location of OneWorld’s clinic, is just under seven hours. The patient that Budine refers to meets with her over Telehealth, but she says that creating follow-up appointments for patients in western Nebraska is incredibly difficult.
“It makes it very difficult for them to obtain any follow up care. For the first year or two, we have to watch labs pretty closely while we’re adjusting medication,” Budine said. “Out in western Nebraska, they either have to drive into Omaha to get labs or find a clinic that I can fax labs to that will then go ahead and get the labs drawn for them and get the labs sent back to me.”
Budine talked about some of the barriers that make it harder for trans people in western Nebraska to obtain hormone therapy.
“It takes a lot of work on [the patient’s] part. Trying to feel safe contacting a clinic and explaining the situation. Usually, they have to make an appointment to go in and there’s some charge. You get into more money because they’re paying to have a visit with me via the phone and them there to have labs. It’s like being charged double,” Budine said.
While most of Budine’s experiences with labs and practitioners in western Nebraska have been positive ones, she reflected back upon a patient she served whose pharmacy made it hard for them to obtain their hormones.
“I had a patient who was out in the Kearney area, and they had originally used one pharmacy. This was a teenage patient, so I was talking with parents. They had used one pharmacy in the town that was giving them a really hard time, so they called and switched to a different pharmacy,” Budine said. “They were not very helpful with insurance and those types of things.”
Sophomore Aiden Whalen explained that even in Omaha, getting labs and appointments to obtain hormone therapy is an incredibly difficult and arduous process for trans individuals.
“I go to UNMC’s clinic for my care. It’s not great. I do all of my meetings online because it is very difficult to get to everywhere in a timely fashion,” Whalen explained. “There was a lot of scheduling issues to where I didn’t have an appointment for nine months, and all of my levels were messed up.”
In Omaha, Whalen said he doesn’t know many practitioners in the state that provide hormone therapy. He said that they attract patients from states in surrounding areas as well, creating a high volume of individuals for a small number of doctors and practitioners able to provide these services.
“Every trans person in Nebraska plus neighboring kinds of places go to these handful of clinics, it’s so swamped,” Whalen said.
The volume of patients that these clinics deal with create problems, such as scheduling errors and missed appointments by clinicians or patients. For patients, this can mean missed hormone prescriptions, missed labs and missed doses. Consequently, patients’ hormonal levels will fluctuate, which brings about side effects.
“I just had a meeting a week ago, and even then, I had one scheduled for two months ago and they didn’t show up,” he explained. “I couldn’t get my lab work done because they wouldn’t set up a time for me to come in and get it done, so I was out of it for like nine-ish months. I don’t blame them for it because there’s only one doctor at my clinic. There are so many people that do it [at UNMC] because we don’t have a surplus of clinics.”
Sophomore Grayson Shuler-Morgan believes that the process of starting hormone therapy is intentionally hard to discourage transgender people, especially transgender youth from starting hormones.
“It’s way too long, the process. I get that they want people to be sure and one-hundred percent ready, but I was ready in 7th grade, maybe 8th grade and I’ve been ready for years and like, they still need to do a whole bunch of assessments and all these appointments that I’m on a long waiting list for,” he explained. “I feel like that’s all to provoke a sense of hopelessness into people – I’ve thought a lot about this – and just make people give up. A lot of people don’t want trans people to be happy, especially here in a red state. It’s just to make people give up, I think. There’s literally no other reason.”
Shuler-Morgan is also disgruntled with the lack of transparency and communication he has received from his hormone specialists. Shuler-Morgan, who is trans-masculine, plans to start taking testosterone at the UNMC Gender Care Clinic in August.
“I’ve heard that they’re overbooked, I’ve also heard that there are not a lot [of practitioners]. I get a lot of mixed messages which also I feel like, it’s just people don’t want me to go on testosterone. I don’t know a lot actually. I just know my experience. I don’t know the facts because people don’t really tell me,” Shuler-Morgan explained. “I’m kinda mad. Like, they’ve just slapped on a waiting period without telling me why or if they have a limit. I’ve asked and they don’t ever give me a solid answer.”
Furthermore, Nebraska requires individuals to wait until the age of 19 to get hormone therapy without parental consent, which can be incredibly taxing for individuals with transphobic parents. An anonymous transgender man (who will be going by X for coherency’s sake) shared his experiences with dysphoria because of a parental reluctance to put him on hormone therapy.
“My parents are transphobic. I was outed to them at a pride parade. My mother told me a few weeks later that ‘I would always be her daughter.’ Unfortunately, due to that, I can’t get on T (testosterone) because I don’t have my parents’ permission,” he said. “I have to wait till I’m 18, and it’s just like, you count down the days, because there’s nothing I can do to change my parents’ minds. You deal with a lot of dysphoria.”
Levi Schiff, a transgender man living in Colorado Springs, CO, touched on some of the effects of being denied hormone therapy.
“It’s had severe effects on my mental health for sure and causes a lot of anxiety and dysphoria,” Schiff said. “A big reason that parents are hesitant about HRT is that the side effects are often permanent, but I’d wish they’d realize that allowing your child to go through a natural puberty is also permanent. Hormone blockers on the other hand are completely reversible and not at all permanent or damaging so as long as you keep an eye on bone density levels and hormone levels, [it’s healthy].”
Mindee Swanson, a Nurse Practitioner at OneWorld, said that for trans patients, it can even be hard to find a primary care physician who they feel comfortable around in rural Nebraska.
She explained that “People think when we say trans care we just mean HRT. Primary care [for trans people] is a big thing too.” Swanson explained that she has “heard some pretty bad horror stories” from trans people about primary care experiences.
Swanson detailed the story of a colleague she had a conversation with. “My colleague (not at OneWord) called me in talking about a trans woman, and she was saying stuff like ‘he gave himself little boobies’ and just having to correct them a bunch of times on this person’s pronouns,” she said. She expressed concern that many trans people may avoid going into a primary care physician’s office because of transphobic experiences, making them more likely to have a disease or disorder go undiagnosed or unchecked for long periods of time.
X said that his experiences with binding have caused uncomfortable experiences at his physician’s office.
“Most people bind until they can have T or get top surgery. You have to be careful with that because you’re binding a chest and that’s where you have all your nerves. People make a lot of risky decisions and I’ve made that mistake myself, which is binding with something that is too small and you can potentially damage the nerves, and I’ve caused myself bruising on my ribs because of it,” he said. “When I’d go to my physician, you’d just see like some bruises sometimes there and like, it’s hard to explain. It’s very awkward to do.”
Whalen said that his primary care pediatrician neglects to answer many of his questions, which causes him frustration because he feels as there are no good sources for him to ask.
“With my primary care they just kind of ignore it, I guess,” he explained. “It’s almost like they’re like ‘maybe if we don’t address it, it won’t be there’ which kinda sucks when like I have questions about stuff that revolves around that like physical activity and all that stuff and they’re just like ‘eh bring it up with your hormone doctor’. But their job is just hormones.”
Whalen also attested to misgendering and deadnaming during a stay at a mental hospital.
“I had to stay in a mental hospital for a while, and Nebraska’s rules are that they can call you by your name, but the name from your birth certificate has to be on your bracelet as well as your sex and they can’t change it unless you go through legal stuff, so that’s what they call you because it’s on your charts,” he said.
Junior Brodie Urwin said that even with his strong support system, his pediatrician and other specialists still fail to use the correct name and pronouns for him.
“My old pediatrician saw that I used he/him pronouns in my chart and didn’t even look at it or address it at all and still misgendered me,” Urwin explained. “I go to Children’s Hospital, and like, they’re okay, they do good with pronouns but sometimes they make it very apparent that they don’t care. My mom will correct them, and I will correct them, and they will continue to use they/them pronouns instead of he/him pronouns and it is very frustrating. If they were to use my correct pronouns, I would feel more comfortable.”
Shuler-Morgan said that even in transgender specific care settings, the environments are uncomfortable because of the lack of trans people in the profession.
“At the gender clinic that I’m doing testosterone at, there is not a single trans person there, which kinda freaks me out. I don’t want my gender journey to be overlooked by cis people, because I don’t really trust them,” he said. “No offense, but they just don’t get it.”
Not only do trans Nebraskans have to deal with transphobia inside of the physical healthcare system, but many trans individuals have had bad experiences with mental health specialists as well.
Shuler-Morgan continued his point about a lack of trans people in professions meant to help trans people. WPATH, the World Professional Association of Transgender Health is a nonprofit that helps identify trans-friendly and LGBTQ+ friendly providers in an area. In Omaha, there are only thirteen WPATH certified physical or mental health providers. While not all trans-friendly providers are listed on WPATH, many make it a point to get certified and approved by them because of the rigorous standards they uphold providers to.
“My last therapist wasn’t exactly, well I’ve had a lot of therapists. I’ve gone through like all of them. My last-last therapist, I had to explain what gender dysphoria was to her,” Shuler-Morgan explained. “She wasn’t anti-trans, she just did not know anything, and she would tell me like ‘that sounds like body dysmorphia’ and like maybe, but it’s body dysphoria. And I just had to explain what I was going through.”
Whalen talked about a series of microaggressions that he has faced in therapy. He explained that a lack of understanding and education is what causes problems within these settings.
“I’ve had therapists say before like ‘I have experience with transgenders’ and I just kinda look at them and I’m like ‘Oh! That’s fun.’ I feel like a lot of it has to do with like if you are transgender a lot of times if you have mental health issues, they think putting you on hormones will solve it all,” Whalen said. That’s not really how that works.”
Swanson explained that the combination of transphobic experiences and lack of access may add on an extra layer of complexity to an already overly complex healthcare scene for trans western Nebraskans.
“There’s definitely a stigma,” Swanson said. “Mental health is a big problem. There’s some statistic that 41% of Transgender Youth have attempted suicide.” She explained that “Finding a [mental healthcare] provider who is friendly” is much harder in the western part of the state.
X believes that it would no doubt be harder to exist as a trans person in the western part of the state.
“I think it’d be a lot harder [to be trans out west]. I live down in Dundee. It’s mixed – you get a lot of liberal people but you also get a lot of right wing people. I haven’t dealt with a lot of bad reactions to it but I can imagine out West it’d be a lot worse. I can imagine it’d be hard to socially transition, and even more hard to medically transition,” he said.
Urwin believes that a lot of problems within the health setting arise from a general lack of understanding of trans people.
“I one hundred percent think that becoming educated and like being willing to be educated is so much of the problem. A lot of people are educated, but they’re not willing to like act upon that education,” Urwin explained.
Sophomore Etta Salzman, a transgender nonbinary person, furthered Urwin’s point.
“Even when we try to inform older generations, they don’t really care,” they explained.
Whalen explained that to make transgender healthcare more accessible in Omaha and surrounding areas, it must be made more visible.
“My clinic is behind a wall of buildings, and the place I went to get my testosterone, I pick it up at a different location, but that one was very tucked away,” he explained. “You can’t really see it. At least having a sign that’s like ‘hey this is here’ because we just circle for a long amount of time and you just kind of give up. If I can’t see it, how can I know that there is something there for me?”
Budine explained that there are not very many accessible and outwardly visible clinics for hormone therapy in Omaha.
“Overall, I don’t think most clinics have that welcoming atmosphere that immediately someone can walk in and feel safe,” Budine said. “When I go to conferences or events where there are other practitioners there, you just talk about ‘what do you do at your clinic?’ or ‘what kind of patient population do you see?’ and you kind of make connections. I always ask ‘are you seeing trans folk? Are you seeing the LGBT community?’ and then kind of get into the conversation of ‘do you have literature? Or a pin on your shirt? Or a rainbow lanyard?’ that you can wear that can make someone feel safe to talk to you. When we do that outreach with other clinics it’s really helpful.”
Whalen talked about the value of being able to ask questions and have a safe space inside clinics.
“It’s such a gut-wrenching feeling to be in the dark about it and you can’t ask questions, and no one really knows and I can’t ask my general practitioner because she just kinda ignores it,” he explained. “I can’t really look it up because a lot of times sources come from very blue states or very accessible states.”
The bottom line is that transgender healthcare is healthcare. There are many barriers across the state, implicit or explicit, that prevent many transgender Nebraskans from receiving the care they need.
Shuler-Morgan explained how he feels that his time is being misspent.
“Yes, they’re like irreversible changes, but people, especially people like me who’ve been out for over a year, well I’ve been out as not cis for three years, that’s enough time to decide,” he said. “The time that I’m in my body that I have been in since birth is like, it’s just wasting time that I could be so much happier, and I think that’s what people want.”
Salzman stated an essential truth.
“Trans people have been around forever,” he said. “It’s just a matter of safety and coming out.”
Whalen wants people to realize that trans people are just that, people.
“We just wanna experience life and live happy lives that we feel fits us best. We aren’t monsters. I’ve been called a monster by full grown adults. I just wanna f**k around and have fun in my high school years and into college. I want to be able to access my care like anyone else would go and access their healthcare. I’d love to be able just to call a doctor and say like ‘hey are my levels messed up’ and they’d be like ‘oh we’ll send you in for a blood test.’ I feel like people need to get their heads out of their a**es and just start researching and asking questions and just realizing that like trans health care, it really is just healthcare, and it doesn’t affect you in the slightest,” Whalen said.
“But it does affect me, and I just want to live a happy life.”
Your donation will support the student journalists of Omaha Central High School. Your contribution will allow us to purchase equipment and cover our annual website hosting costs.

Hi! My name is Charlie (he/him), and I'm a senior. This is my fourth (and final </3) year on staff, and I’m the Co-Editor-in-Chief. I was voted most...